Scalp Conditions
The aim of a Clinical Trichologist is the diagnosis and treatment of diseases and disorders of the hair and the scalp.
It is surprising how many conditions this embraces, ranging from dandruff (pityriasis capitis) and seborrhoeic dermatitis to fairly rare genetic disorders and the consequences of endocrine dysfunction.
Seborrhoeic Eczema
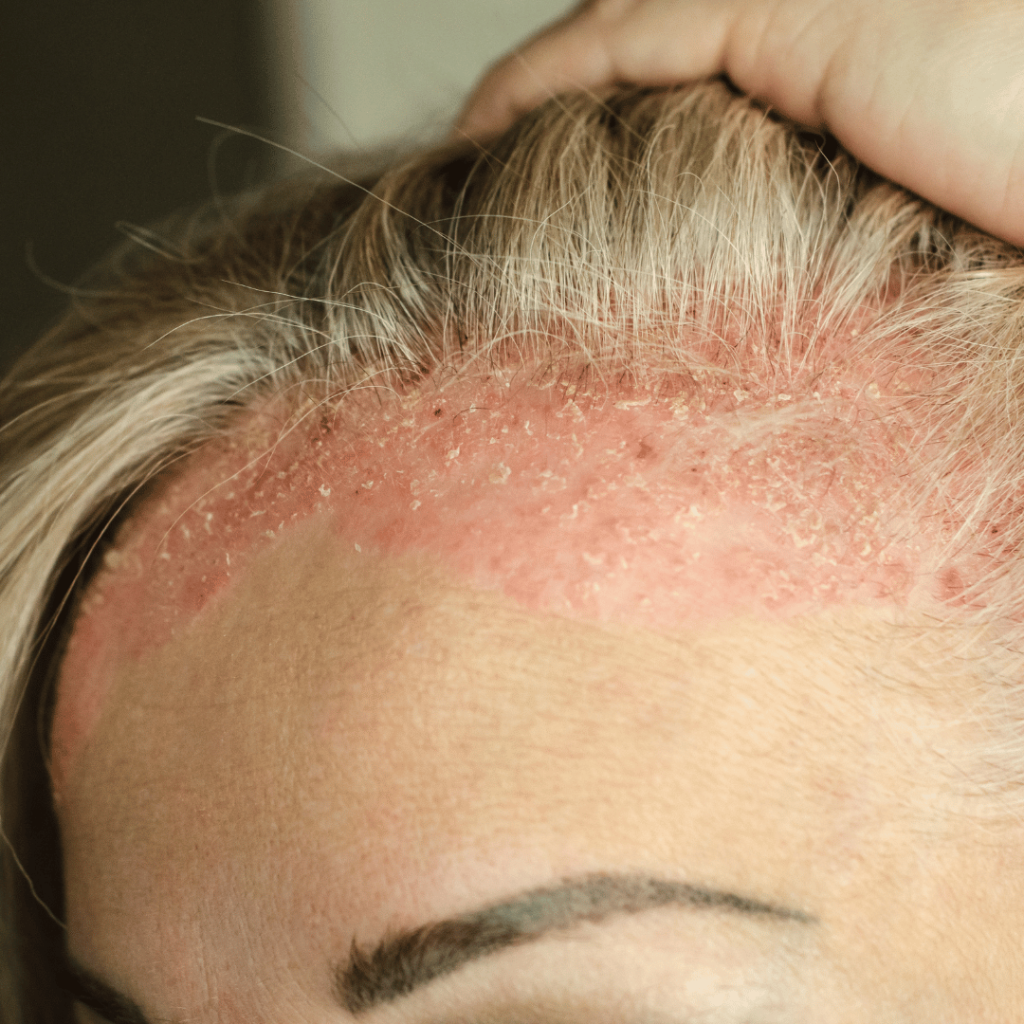
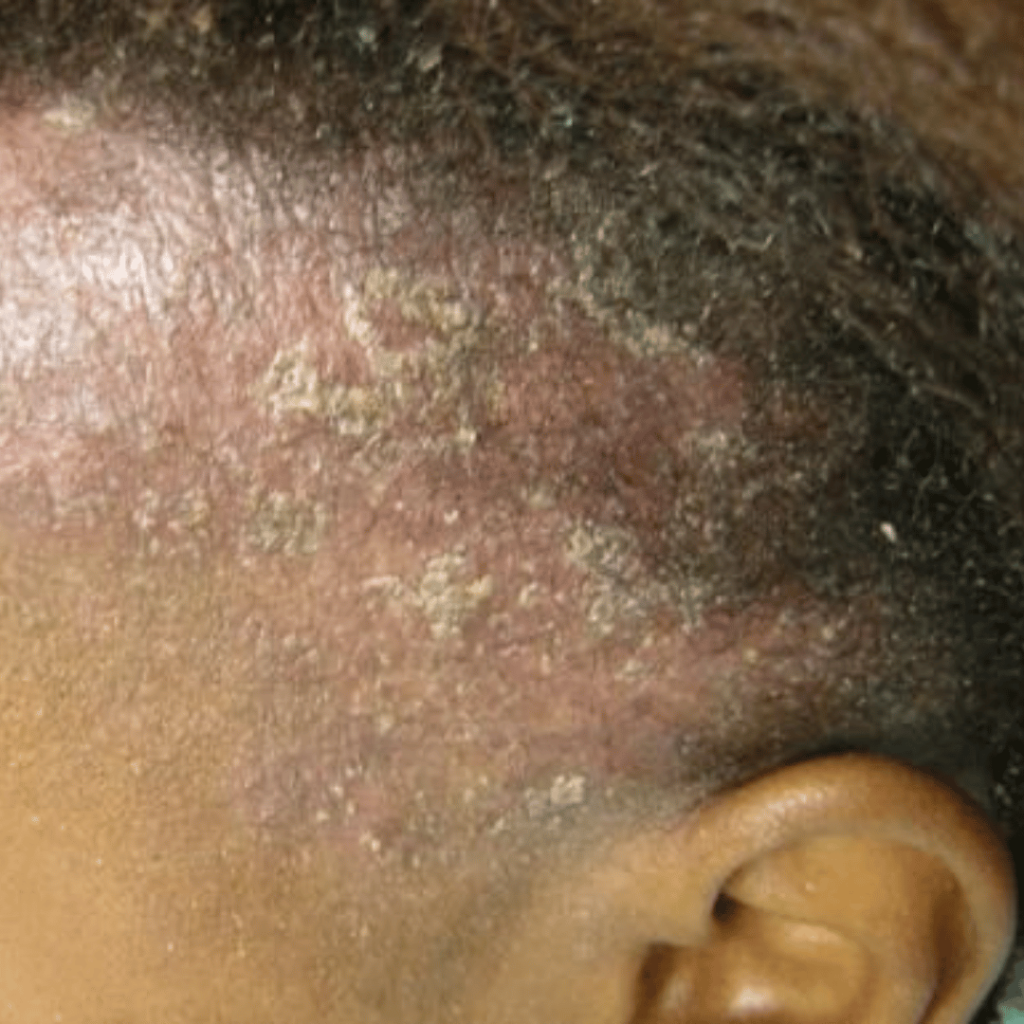
Seborrhoeic eczema is a chronic relapsing inflammatory scalp condition occurring in seborrhoeic areas (areas with more sebaceous glands). It spite of the name it is not necessarily an oily condition. It presents differing signs, varying between mild pruritic scaling and erythema, to excessive scaling and crusting formed from dried exudation over a red and moist scalp.
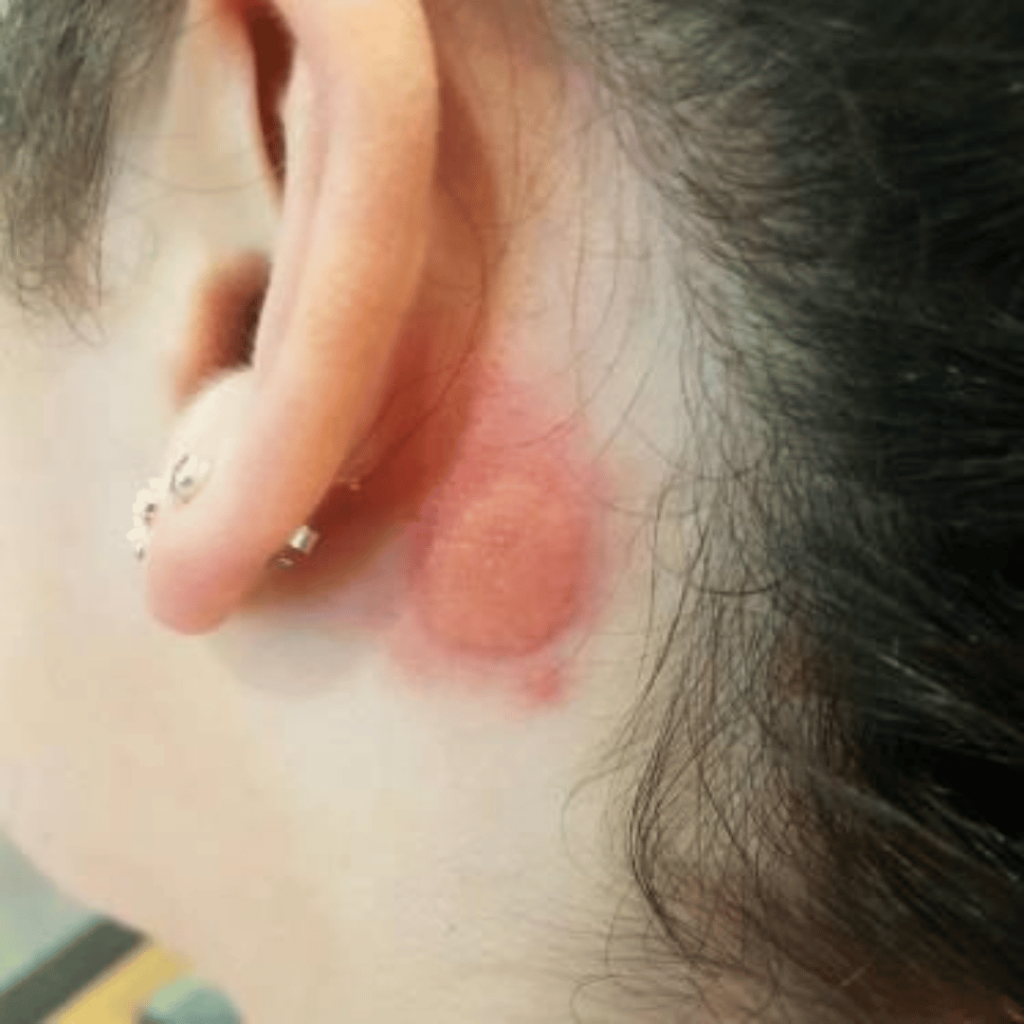
The whole of the scalp can be affected, particularly the margins and retro auricular area behind the ears. Seborrhoeic eczema can be highly pruritic, which leads to excoriation and secondary infection with pustulation. Seborrhoeic eczema occurs in infancy as cradle cap and is rarely seen throughout childhood. It returns at puberty or later and lasts throughout life. Infantile and adolescent forms are likely to be two distinct conditions.
Irritant Dermatitis (Contact Dermatitis)
Irritant dermatitis is caused by a substance which can create cell damage when applied for the first time in strong concentrations i.e. bleach, relaxer (sodium hydroxide). It can also occur when weak concentrations of successive applications i.e. shampoo are used. That substance is called the primary irritant. The reaction caused may be inflammatory but it is not an allergic reaction.
Primary irritants that may cause non-allergic reactions include shampoos, hair cosmetics such as conditioners, setting lotions, or perm lotions, para-dyes and relaxers on black hair. Plants and metals can also create similar problems.
Allergic dermatitis (Contact Dermatitis)
Allergic dermatitis is a potentially life-threatening reaction to a substance previously used on the skin. The reaction takes place some time later. The allergic reaction creates an intensely irritable reaction, which happens after a substance has been applied to the skin.
A few hours or even days after the application of the substance, the affected skin may become swollen, red and blistered or dry and crusted. Mostly the area in contact with the substance is affected but when the scalp is affected, the reaction can spread to the eyes and face and sometimes there can be swollen lymph nodes and secondary infection. There can be anaphylactic shock with subsequent restriction of the windpipe. Allergic dermatitis causes intense itching and burning.
Psoriasis
Psoriasis often begins on scalp or elbows with circular areas of uniform darker/ redder skin clearly differing in colour from adjacent normal coloured skin. These areas are covered with dry white, adherent silvery scales, which can sometimes be quite dense. These scales are not easily removed but when they are, then coarse lined skin with bleeding points can be seen underneath them. Other areas that can be affected are the knees, elbows and shins. The fingernails and toenails can be affected with thimble pitting. Stiff and painful joints can accompany psoriasis.
The cause of psoriasis is unknown, but there would seem to be a familial trait. Two per cent of Caucasians suffer from the condition, which more commonly appears between the ages of ten and thirty. The condition is triggered by stress, skin damage, illness and bacterial infection. Itching to an adjacent area often denotes an extension of the condition.
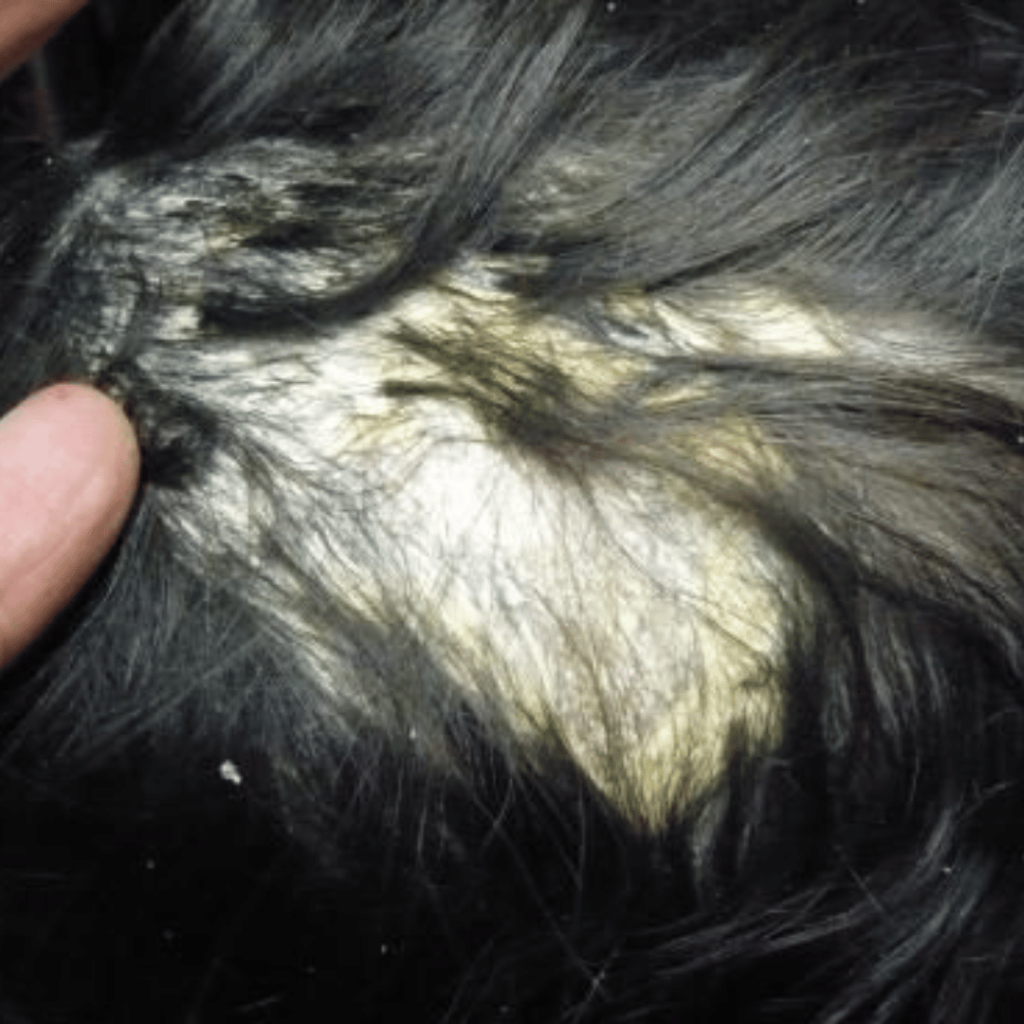
Pityriasis Amiantacea
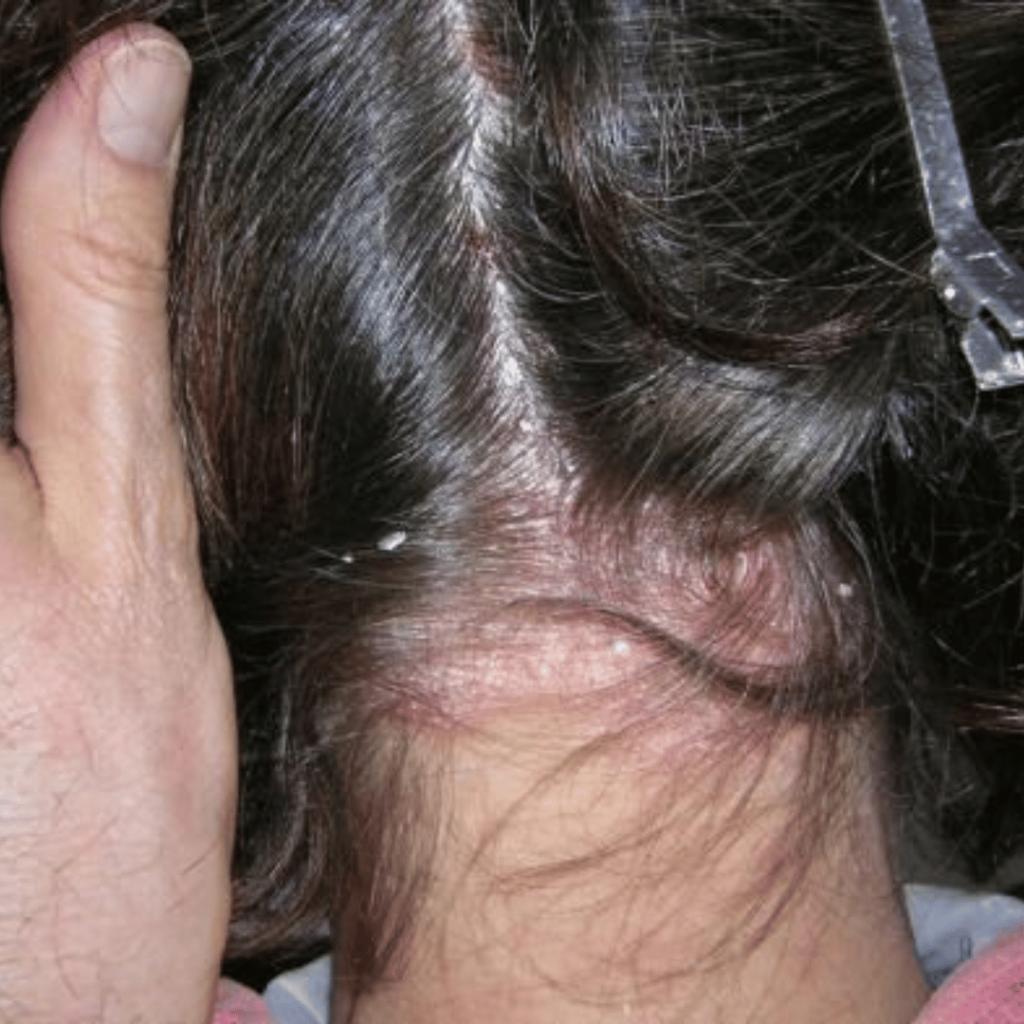
Pityriasis amiantacea presents one or many areas of heavy, sticky scales, built up along the hair shaft most often situated at the crown and parietal area. There is an eczematous reaction of scalp to trauma, infection, or idiopathic which follows weeping to the area. There are thick asbestos-like scales firmly adhering to scalp and along hair shaft like tiles on a roof. It rarely covers the whole scalp.
Pityriasis amiantacea usually follows a period of intense emotional stress or a localised streptococcal/staphylococcal infection. The area may weep at first followed later by thick, smelly, sticky scales. Often there is a habit factor involved with an itch-scratch cycle being established. The sufferer may try to scratch away the heavy scaling even when it is not pruritic. Scratching or picking at an area causes a divot of hair-bearing scalp to be removed causing temporary hair loss to the area.